PAIN-FREE MANAGED MEDICAL BILLING
Focus on Patients, Not Billing
Pain-Free Billing
Medical billing is a major component of every medical practice. In this age of reduced
reimbursements,
getting paid on time and accurately is a priority. Choosing
the right billing
service is incredibly important. We are confident that once you learn about our capabilities,
DrChrono will be
your billing service of choice. Please read on to learn about our Managed Billing Services.
End-to-End Billing Management Lets Providers Focus on
Patients
We believe that providers should spend their time
caring for patients, not chasing down payments.
DrChrono’s integrated EHR lets our billing team
take over as soon as a provider completes patient
charting.
-
Real-time eligibility verification at the time of patient check-in: we educate and train doctors and their staff to utilize this feature effectively in order to collect payments up front.
-
Experienced and certified medical coders: our coders review clinical notes and code them with the correct ICD9 and CPT codes. Additionally, we coach doctors on appropriately optimizing charting for claims.
-
Excellent clean claim submission rate: our billing team reviews all claims before they are submitted to insurance in order to increase a provider’s first time payment ratio. Our clean claim submission rate is above 98%!
-
Comprehensive front-end rejections process: our senior billers review and re-submit rejections within 48 hours. Additionally, our team works closely with clearinghouses and insurance companies in order to get your claims paid on time.
-
Expert Electronic Remittance Advice review: our billing experts review all payments to ensure proper reimbursement per doctor contracts. Additionally, the team ensures that payments are appropriately deposited in the doctor’s bank account.
-
Speedy accounts receivable follow-up and collections: our team follows up with insurance companies immediately as opposed to the standard method of aging claims. This allows us to recover payments quickly; in fact, more than 96% of our claims are paid in less than 60 days!
-
Specialty-specific denial analysis, resolution and prevention: we are well-versed in denial resolution by specialty. To ensure most claims are paid without a denial, we monitor denials for trends. We then train and educate your team to make appropriate changes in their workflow to reduce future insurance denials.
-
Multi-Insurance appeals specialization: we have extensive experience across all kinds of appeals, including those for federal, commercial, workers compensation and auto insurance.
-
Accelerated patient statements and follow-up: our team sends statements in a more timely manner than most standard billing operations; this helps practices recover receivables faster. Additionally, we contact patients after sending statements to ensure on-time payments.
-
Simplified credentialing: our services include credentialing, re-credentialing, contract negotiations, malpractice application submissions, and network participation amongst other things. Our goal is to simplify the process and reduce the costs and frustration associated with credentialing.
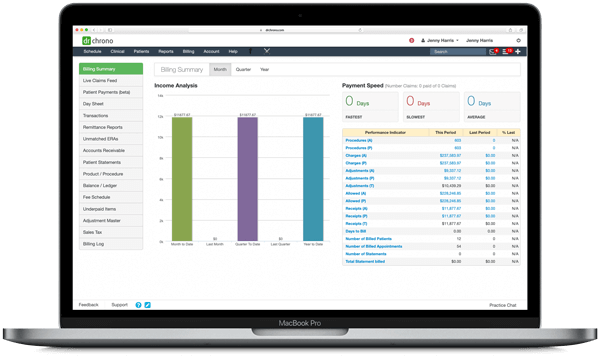
Completely Analytics Give You Full Cash-Flow Insights
Just because a practice’s billing is outsourced
doesn’t mean that providers need to be in the
dark on on billing activity, cash flow, and other
key billing measures. The DrChrono reporting
center gives our providers an easy way to
understand their billing.
Our reporting center can be accessed in one click via the DrChrono EHR; reports are easy
to understand, up-to-date and incredibly
powerful in allowing a provider to understand a
practice’s financials.
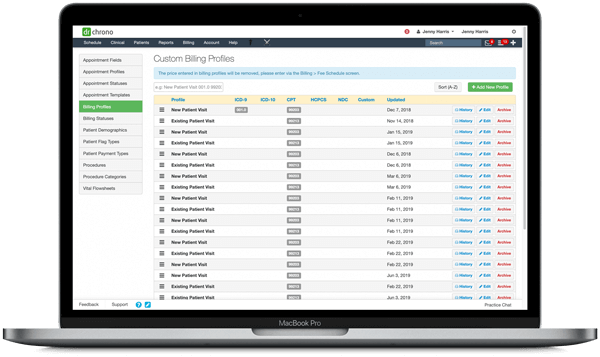
Completely Integrated EHR & Billing Provides
Visibility
Some EHR’s offer billing services, however
most systems are not integrated between
EHR and billing systems. This means providers
have no visibility into their own billing. Our EHR
was built-in tandem with our billing system
in order to ensure that both the EHR and
billing system are seamlessly integrated. This is
significant for three reasons:
-
Doctors and their designated staff have 24/7 access to billing statistics and analytics. With the click of a button on the DrChrono EHR, doctors can view easy to understand snapshots and reporting of payments, denials and cash flow.
-
Billers have access to patient charts, which is invaluable in boosting practice revenue. With an integrated system, billers can easily analyze charting and work-flow practices and quickly advise a provider or their staff on modifications needed to optimize billing outcomes.
-
Patients have online access to their medical records. Thanks to our integrated system, patients are able to log-in to our patient portal, OnPatient.com, and see their clinical summary, book appointments and view and pay their statements online.
Our integration also permits us to utilize the
expertise of our in-house Coding Compliance
Officer who reviews all provider clinical
documentation in order to ensure providers
meet required compliance levels. This is a key
initiative as it ensures that all clinical
documentation meets or exceeds insurance
company and Medicare guidelines. This also
prepares practices to easily pass audits,
particularly Medicare’s audit.
Dedicated Team of Billing Experts
An effective billing team is the backbone
of a practice. DrChrono assembles a billing
team per practice; each team is based on an
individual practice’s needs and specialty.
Additionally, each team member is an expert
in billing. As a rule, each of our billers has at
least 4 years of hands-on experience with
single if not multiple certifications in coding,
auditing and billing.
Our billing team is especially unique in that
our coders are managed by a medical doctor
who ensures that provider perspective and
logic is integrated into our billing workflows.
Best of all, this team is very accessible - they
can be contacted easily via a dedicated toll-free number and email.
-
CPC: Certified Professional Coder (Physician Practice)
-
CPC – H: Certified Professional Coder – Hospital Outpatient
-
CPC-P: Certified Professional Coder - Payer
-
CPCO: Certified Professional Compliance Officer
-
CPMA: Certified Professional Medical Auditor
-
CGSC: Certified General Surgery Coder
-
CASCC: Certified Ambulatory Surgical Center Coder
-
CPB: Certified Professional Biller
ICD-10 Ready To
Ensure No Billing
Gaps in ‘15
The new ICD-10 standard changes coding
significantly. ICD-9 had
approximately 18,000 codes, while ICD-10 has
nearly 65,000.
This new standard is incredibly challenging
to learn, however our billing team has been
prepared and ready for ICD-10 since we learned
of its proposed use nearly 5 years ago. This is
a major advantage for our clients because we
mastered ICD-10 ahead of the curve and have a
cohesive strategy for working with this coding
system.
Fair Fee Structure
Lets Practices
Retain More of
Their Earnings
Our fee structure is flexible and allows us to
offer our services to practices of all sizes.
Our pricing is structured simply:
-
We assess a percent-based fee monthly based on the amount of billing we process for your practice. The higher your billings, the lower your fee.
-
Our fees range between 3-8% billed monthly. We bill the greater of an agreed upon minimum fee or the % fee. Of course, we can create a custom plan for new and smaller practices.
Certified to Bill Professionals and Institutions
Our flexibility to bill professionals and institutions makes us the biller of choice
for individual practices as well as surgery centers, labs, and certain specialty
out and in-patient centers.
Specialty Specific Billing
Capabilities
Specialties require a high level of practice
specific billing knowledge in order to bill
most efficiently for all procedure and
appointment types. DrChrono’s billing team
has specialty-specific experts on board such
that we can optimally bill for any practice. In
fact, our billing specialists are certified in all
major specialties, including:
-
Anesthesiology
-
Cardiology
-
Dermatology
-
Gastroenterology
-
Immunology
-
Obstetrics-Gynecology
-
Pediatrics
-
Plastic Surgery
-
Pulmonology
-
and 85 more specialties…
A Profitable Story
DrChrono’s managed billing services have
helped thousands of our clients increase their
revenues dramatically.
One illustrative example is that of a Boston-based family practice that grew their revenues
significantly after adopting DrChrono, without
any change in appointments or number of
clients.
DrChrono’s billing team is able to provide clients
with significant revenue improvements for two
reasons:
-
We are able to collect a greater amount of your billings than most in-house or specialty billing companies
-
The cost of our services is far lower than what most providers pay an in-house biller or billing company
Before: In-House Biller
| Total Insurance Eligible Billings per Month: | $26,000 |
| Total Amount Collected per Month via an In-Houre Biller: | $18,200 |
| Total Monthly Cost of In-House Biller (includes benefits): | $6,176 |
| Total Annual Collections, Net Cost of Biller | $144,288 |
After: DrChrono's
Managed Billing Services
| Total Insurance Eligible Billings per Month: | $26,000 |
| Total Amount Collected per Month via an In-Houre Biller: | $22,100 |
| Total Monthly Cost of In-House Biller (includes benefits): | $1,820 |
| Total Annual Collections, Net Cost of Biller | $243,360 |
Revenue Improvement with DrChrono: $99,072
CASE STUDY:
BILLING & EHR
Chiropractor
Theif River Falls, Minnesota
“DrChrono’s managed billing services
were critical in taking my practice to the
next level. I was absolutely blown away
by the billing team - I no longer had a
single person supporting my billing, but
an entire team dedicated to helping me
succeed.
”
Practice Background
Shortly after completing Chiropractor’s
College, our client started a practice in
Thief River Falls, Minnesota. Like many
new practitioners, he was entirely new to
the world of billing. As our client puts it,
“they don’t teach you billing in school...
any school.”
"My revenues quadrupled
after adopting DrChrono’s
EHR billing services."
Billing Challenge
With no experience in billing, our client
hired a biller, who was an expert*
in billing for chiropractic. After some
time, our client noticed that he had
an abundance of new patients and
appointments, but he was seeing very
little revenue from his billings. Since
our client was already a DrChrono EHR
customer, he called DrChrono for help.
Results of Implementing DrChrono's Managed
Billing Solution
DrChrono set our client’s practice up for
success. He was immediately set up with a
team of billing specialists who overhauled
his billing practices...all at a lower cost than
what he was spending for his internal biller.
The results speak for themselves:
| Before | DrChrono | |
| Claim Submission | 20-25% | 100% |
| Claim To Payment Time | 4-6 weeks | 1 week |
| Cashflow | Poor | Excellent |
| ROI on Billing Services | Negative | 3900%* |
| Gross Revenues | 4X Improvement | |
*ROI formula ((revenue gain - cost of services)/(cost of
services))
"DrChrono provided EvoFoot with scale
that no in-house biller or billing company
could have provided us. It’s a no brainer –
clear your office of your billing headaches
and have DrChrono manage your billing
instead. Just sign the dotted line!"
– Dr Ali Sadrieh, Foot Surgeon - EvoFoot, Studio City
DrChrono helps nearly 70,000 doctors
and 3 million patients
with their electronic health records and billing needs. DrChrono recently was added to the
Inc. 500 list of the fastest growing companies
in America and in an independent survey of over 22,000 doctors, was
voted #1 EHR for iPad two years in a
row.
Interested in learning more? Please
contact us to set up a demo of our
advanced billing services.
